Here you can find key information related to reimbursement claims and doctor’s and hospital bills.
Where do I send reimbursement claims if I have already paid a bill myself?
You should send reimbursement claims or the original bills to your ÖKK agency. Or it’s even easier if you use the myÖKK customer portal.
You can use the myÖKK app to send the bills and invoices to ÖKK directly. You will then be refunded the costs less the cost-sharing amount (annual deductible and excess).
myÖKK App – simple, quick and clear


Do I have to first of all pay a doctor’s or hospital bill myself and then send it to ÖKK or the other way around?
When the bill is issued, you have to pay it yourself. Send ÖKK your reimbursement claim or the original bills as quickly as possible.
We recommend that you only pay your bills once you have received a reimbursement from us. This helps us challenge service providers (medical specialist, hospitals etc.) if we believe they have billed an excessive amount. In this way, we can together avoid you paying more than necessary.
If we do not have your account details, please provide us with bank or post office account details.
Why might it be that ÖKK has not yet reimbursed my bill?
Your cost contribution (annual deductible and excess) are deducted from the bill amount for as long as your deductible and excess have not been used up. If the bill amount is less than your annual deductible, you do not receive a reimbursement, but instead a statement for your information. There you can see that the bill amount has been deducted from your deductible and how much of your annual deductible is remaining.
I have my basic and supplementary insurance policies with different health insurers. How do I settle benefits with two insurance policies?
- Make a copy of the doctor’s or hospital bill.
- Send the original bill to the health insurer with whom you have your compulsory basic insurance.
- The health insurer then settles the benefits from the basic insurance policy.
- Compare the benefit statement you received with your doctor’s or hospital bill.
- If certain benefits have not been covered by your basic insurance, send a copy of the bill and a copy of the benefit statement to the health insurer with whom you have your supplementary insurance.
- If benefits are covered by your supplementary insurance, the health insurer will settle these and you will receive another statement of benefits.
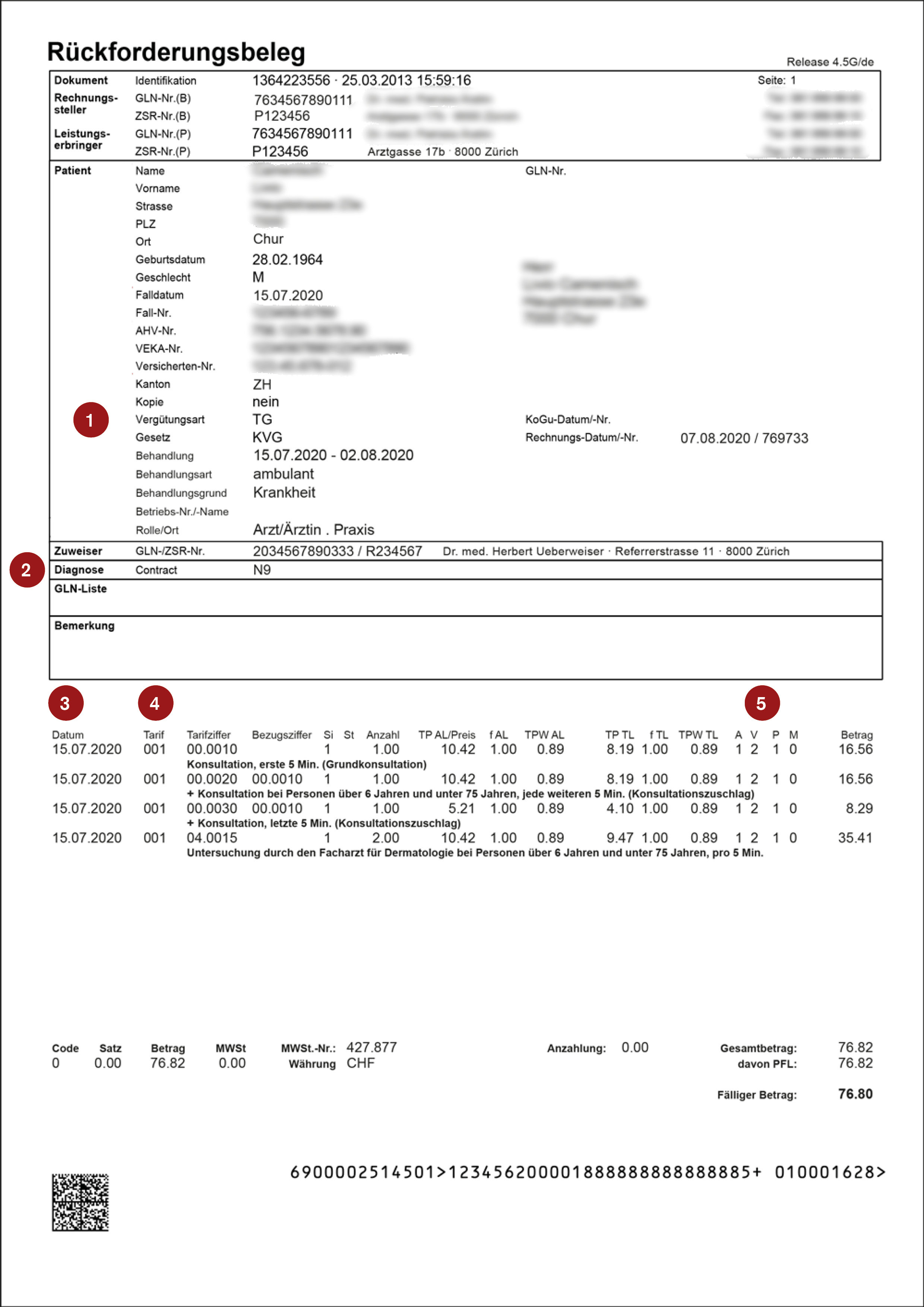
How do I check my doctor’s and hospital bill?
It’s easy to understand why anyone who is not an expert might need help checking bills from doctors or hospitals. We can explain how to decipher the codes.
1 Type of reimbursement
TG stands for “Tiers garant”: This means you pay the bill and then send a reimbursement claim to your health insurer.
TP stands for “Tiers payant”: The invoices are sent directly to your health insurer. You only receive a statement of benefits. As a policyholder, you are entitled to receive a copy of the invoice from the service provider if this is processed under TP.
2 Diagnosis
The diagnosis is recorded using the “Tessiner Code” or “ICD-10” and only provides a very broad description of the condition.
3 Date
Did you receive treatment on this date? Please note: Telephone consultations are also invoiced as well as other services that were provided in the absence of the patient (e.g. studying medical records).
4 Tariff
The benefits are split into various tariffs.
The most common are “001” for doctors’ services, “402” for medication and “317” for laboratory analyses.
5 Mandatory benefit codes (P)
If this is “1”, basic insurance covers the costs (PFL = Pflichtleistung = mandatory benefit); if it is “0”, it does not (NPFL = Nicht-Pflichtleistung = non-mandatory benefit).